In medical billing, eligibility verification is also a critical front-end process that establishes the insurance cover, benefits and financial obligation of a patient prior to the provision of healthcare services. It also makes sure that the policy of the patient is valid and the intended services are covered by the payer to prevent the unnecessary billing problems. With in advance verification of eligibility, the healthcare organizations can set correct expectations regarding the reimbursements and the payment of the patients.
Confirmation of insurance prior to the provision of services is crucial in reducing claim denials, delays in payments, and patient unexpected balances. Once eligibility is verified in advance, providers have an easier insurance eligibility verification process in claims and better cash flow as well as having less administrative work up. Simultaneously, patients enjoy an increased level of transparency on their coverage and out-of-pocket expenses, which results in a more favorable overall healthcare experience. This blog will try to explore the eligibility verification process in medical billing step by step.
What Is Eligibility Verification?
Eligibility verification process in medical billing is the part of the process, which involves the systematic review of insurance eligibility of a patient, coverage and benefits of a patient before healthcare services are offered. It verifies the presence of active medical insurance of the patient and determines which of the covered and non-covered services, co-payments and deductibles, coinsurance exist.
This eligibility and benefits verification process in medical billing, commonly known as what is eligibility in medical billing, is beneficial in making sure proper medical billing, minimizing revenue leakage, and reinforcing revenue cycle management (RCM) by making sure that claims are made properly the first time. Medical practices can improve eligibility verification process through outsource medical billing services.
Eligibility Check vs. Preauthorization
Although the eligibility verification process in medical billing ensures that the insurance eligibility and benefits are secured, it does not equal the previous authorization. Eligibility checking in medical billing is concerned with the active nature of the patient health insurance and the benefits whereas prior authorization is concerned with whether payer approval is needed on the specific CPT codes or HCPS codes based on medical necessity.
The two processes are both vital in the healthcare eligibility verification process but benefits verification, which is often the initial process to prevent eligibility related denials and billing delays.
When Eligibility Verification is to be Done
The eligibility verification process in medical billing should be carried out in the pre-visit checking, preferably at the time of the schedule and before the service date. Insurance eligibility verification at such stages enables front desk and billing personnel to ensure that there are coverage effective dates, plan type (HMO, PPO, EPO), and financial responsibility of a patient.
Eligibility verification related to insurance enables a healthcare provider and medical billing company in the USA to make clean claims, increase the rate of claim acceptance, and provide a clear and transparent patient experience by verifying coverage, benefits, and financial responsibility before the service is provided.
Pro Tip: Perform eligibility verification at both scheduling and pre-service stages to catch coverage changes early. Partnering with a reliable medical billing company can further ensure accurate checks, reduce claim denials, and improve revenue cycle efficiency.
Why Eligibility Verification Matters in Medical Billing
Eligibility verification process in medical billing as it helps to avoid claim denials and rejection on an inactive coverage, wrong policy details, or non-covered services. By the verification of eligibility process in medical billing being done prior to rendering of services, the billing teams will be able to realize the coverage limits, referral needs and benefit exclusions before the services are rendered. This proactive strategy will greatly curb the denials through eligibility and also aid in the lodging of clean claims to insurance payers.
Moreover, proper eligibility check during medical billing allows proper patient billing and subsequent reimbursement of the payment to the patient by clearly specifying co-payments, deductibles and coinsurance. Upon confirmation, the healthcare providers save on rework, follow-ups and manual corrections to save on the overall administration load. This lean process enables the billing units to concentrate on financial efficiency in the revenue cycle and enhance the financial experience of the patient.
Benefits of the Eligibility Verification Process
The eligibility verification process in medical billing provides healthcare providers with a huge benefit both operation wise and in terms of financial benefits. Ensuring insurance eligibility and benefits early would decrease denials, enhance accuracy in reimbursement, and reinforce total revenue cycle management and ensure a clear patient financial experience.
Reduced Claim Denials
Medical billing checks the eligibility of active insurance, effective dates of insurance cover and services to be covered prior to treatment. This will avoid eligibility-based rejections due to lapsed policies; procedures not covered or wrong subscriber data provided to the insurance payers.
Improved Cash Flow
Proper check on insurance eligibility helps insurance companies to make quick claims and promptly settle their claims. The timely manner in which healthcare providers are paid and payment delays and revenue leakage across the revenue cycle are minimized when eligibility and benefits are checked in advance.
Accurate Patient Billing
Eligibility verification processes in medical billing have indicated clearly the copayments, deductibles, coinsurance and maximum out of pocket. This will enable the billing departments to produce the correct statements to the patient and eliminate conflict arising due to lack of proper insurance benefits verification.
Improved Patient Contentment
Healthcare eligibility verification enhances transparency because it ensures that the patient is informed of their insurance coverage and liability prior to the provision of services. Effective communication fosters trust, lowers the chances of bills being disputed, and enhances the overall experience of patients in medical practices and clinics.
Operational Efficiency
Eligibility verification for insurance coverage is automated to minimize manual follow-ups, rework, and billing errors. The front-end process streamlines billing and registration functions to enable staff to concentrate on clean claims, as well as accounts receivable management services to minimize delays in payments and follow-ups.
Compliance Support
Eligibility verification process in medical billing helps to adhere to payer policy, HIPAA regulations and insurance requirements. Effective reporting of coverage checks and benefits assists medical professionals to comply with audit and regulatory requirements.
Under HIPAA, HHS has established standards for electronic eligibility and benefit inquiry and response transactions, which enable healthcare providers or health plans to request and receive enrollee eligibility and coverage information electronically from health plans.
Improved Revenue Cycle Management
Benefits Checks and Verification of eligibility make the front-end of the revenue cycle management more sound as the coverage is properly checked prior to the care delivery. This is a proactive solution that enhances the rate of claims acceptance, lowering the denials and maximizing financial performance of the healthcare providers.
Information Required for Eligibility Verification
Eligibility verification process in medical billing is anchored on accurate data collection. Full and accurate information will enable healthcare providers to check the insurance eligibility, benefit and coverage details with efficiency to prevent denial of claims.
Patient Demographics
Demographics of the patient entail the complete name of the patient, date of birth, gender, address, and contact information. Proper demographic information will assure proper identification of the patients and avoid error in eligibility verification due to inaccurate recording with the insurance payers.
Insurance Policy and Group Number
The patient has health insurance which is defined by the insurance policy number, and group number. The information is crucial in the eligibility verification of insurance and helps the payers to access accurate information regarding the coverage and benefits.
Subscriber Information
Subscriber data comprises the name of the policyholder, his or her relationship with the patient, and date of birth. Such information is essential in cases when the patient is a dependent, and contributes to proper insurance benefits checks.
Provider and Service Details
The information about providers and services covers the name of the healthcare provider, his NPI, location, and intended services or CPT codes. This data assists in the verification of network status, services covered and benefit restrictions in the process of eligibility.
Pro Tip: It is always important to verify patient demographics and insurance information for accuracy to prevent denied claims. You also need to keep subscriber information updated, particularly for dependents, to verify benefits accurately. Lastly, verify credentials and service codes prior to submission to ensure coverage and network eligibility.
Step-by-Step Eligibility Verification Process
The eligibility verification process in medical billing ensures that healthcare providers check insurance cover, patient benefits, and financial responsibility prior to service. The process of claims is minimized after every step, ensures the simplification of the billing process and enhances management of the revenue cycle.
Step 1: Gathering of Patient Data
Record patient demographics, such as full name, date of birth, contact and insurance information. Proper information at the scheduling or registration enables one to do insurance eligibility validation and avoid mistakes and cover checks are done easily with the payers.
Step 2: Check Insurance Cover
The Medicaid and CHIP eligibility verification systems are now dependent on trusted electronic sources of data, including the Social Security Administration and the Departments of Homeland Security and Labor, rather than paper-based documentation from the patient. As part of the insurance eligibility verification process, the healthcare provider determines whether the patient’s health insurance is active or inactive, as well as the dates of effective and terminated coverage. This is part of the verification process to ensure that the patient has the right health insurance or government programs, such as Medicare or Medicaid, to qualify for the next healthcare service.
Step 3: Confirm Covered Services
Check the services covered by the plan such as in-network and out-of-network benefits, exceptions, and restrictions. Verification of proper insurance benefits will guarantee that the procedures, CPT codes, and services provided to the patient are covered by their policy, and they are less likely to face a claim denial.
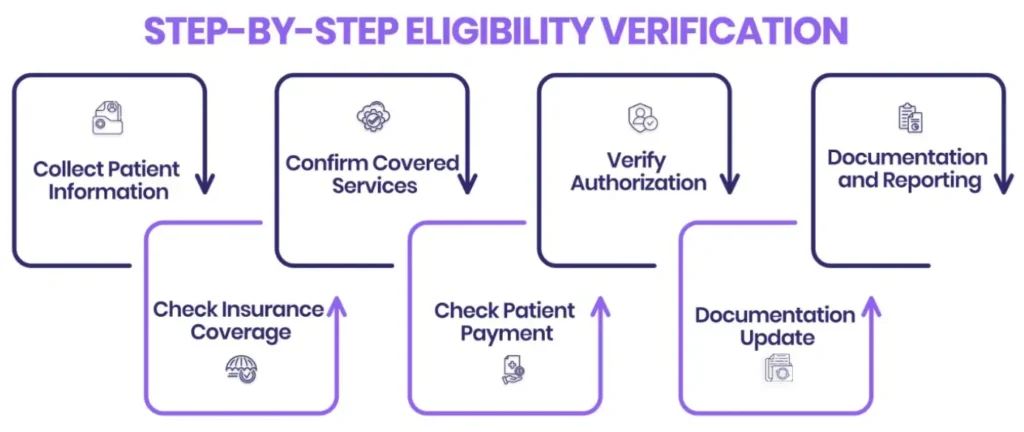
Step 4: Check Patient Financial Responsibility
Identify copayment, coinsurance, deductible and maximum out of pocket payments of the intended services of a patient. The direct payment of a patient is confirmed at the eligibility and benefits verification stage which assists the health care service provider to convey the correct costs and avoid billing shocks.
Step 5: Identify Referral or Authorization Requirements
Establish whether a referral by a primary care physician or previous approval of the insurance payer is required. Verification of medical necessity and payer policies will ensure that every requirement is met and prevent delays in reimbursement of claims.
Step 6: Document and Communicate Verification Results
The verification information, including status of coverage, benefits, and patient responsibility, should be noted in the practice management system or EHR. It is important to communicate the estimated costs to the patients, which will help in a smooth revenue cycle and will also be in line with best practices that emphasize the importance of outsourcing DME billing services to increase the revenue management of your practice.
Pro Tip: Eligibility checks should be done at the time of booking and the day prior to the date of service to ensure that last-minute changes in coverage are identified and claims can be submitted successfully. The use of automated eligibility tools and mature billing partners will further enhance accuracy and cash flow and revenue cycle performance.
Methods of Eligibility Verification
Medical billing can conduct eligibility verification using several different techniques all aimed at ensuring that insurance cover and benefits of the patients are verified in an effective manner. Manual verification would be to make calls to insurance payers directly on phone or through payer portals to verify active coverage, type of plan and benefit information.
Electronic verification employs the EDI transactions, including the ANSI X12 270 eligibility inquiry and 271 responses to obtain real-time insurance eligibility and benefits in a fast manner. Moreover, the clearinghouses and practice management systems make the process more convenient with automated eligibility checks, lowering the administrative load and increasing the accuracy of the revenue cycle management process.
Common Challenges in Eligibility Verification
There are a number of challenges that can impede effective eligibility checking in medical billing and affect accuracy of claims, billing patients, and efficiency of revenue cycle. Identifying these barriers assists the health care givers in using measures to minimize the denials and making the procedure of enquiring insurance benefits easier.
Wrong or Inaccurate Patient Data
The absence of patient demographics or misleading patient demographics may cause a hitch in the insurance eligibility process. Billing and front desk employees have to make sure that they do not miss any data during registration to avoid the denial of claims and delays in coverage.
Insurance Plan Complexity
The insurance benefits verification can be complicated because of the variety of insurance plans with different coverage rules, exclusions, and network requirements. Medical professionals are to be aware of the policies of each payer, such as government, commercial and managed care plans, to be able to check the eligibility of patients and services covered.
Last-Minute Eligibility Changes
Policy changes, termination or switching plans may alter insurance coverage without any prior notice. This kind of last-minute changes in eligibility makes healthcare eligibility verification tricky and would have to be checked in real-time to prevent the filing of claims in the services that are inactive or do not get covered.
Limited Staff Training
Medical billing requires adequate training of front desk and billing staff in the process of verifying eligibility and benefits which will result in errors and inefficiencies. Education of the staff also makes the verification correct, minimizes administrative load, and facilitates the maintenance of revenue cycles.
Best Practices for Effective Eligibility Verification
Accurate eligibility verification goes beyond basic insurance checks it requires a deeper understanding of payer rules and complete laboratory billing guidelines that directly impact claim approval. When healthcare providers align eligibility verification with these guidelines, they reduce costly denials, strengthen accounts receivable performance, stabilize cash flow, and create a smoother, more transparent financial experience for patients.
- Carry out pre-visit verification to ensure active insurance, coverage, and benefits to minimize claim denials and to guarantee proper billing.
- Install EHR or practice management systems that have real-time eligibility checks to simplify the process of verification and reduce the number of manual errors.
- Train employees on insurance cover, and payer criteria and benefit claims to enhance accuracy and efficiency.
- Document all verification findings, coverage, and responsibilities of money by patients to be used in compliance, audits and future reference.
- Verifying provider network involvement is essential to cover services and avoid negative surprises on the part of patients.
- Make patients aware of copayments, deductibles and coinsurances to be paid before services are provided.
- Re-check insurance cover on repeat visits or prolonged treatment to take into consideration the alteration or cancellation of the policy.
- Special plans, government insurance or managed care may be covered by individual contact insurance providers which is why it is important to inquire about benefits verification.
- Streamline workflow with batch eligibility check of multiple patients and real time checks of urgent visits or same day visits.
- Periodically assess the eligibility workflows and the denial reports to detect the gaps and enhance the overall management of the revenue cycle.
Pro Tip: Automated eligibility check tools need to be combined with frequent staff training to make sure that every check is correct, to minimize the denial of claims, and to enhance AR in the medical billing process. Regular tracking of workflow and denial reports can maximize cash flow and enhance the process of controlling the entire revenue cycle.
Consequences of Skipping Eligibility Verification
Omitting the procedure of eligibility verification used in medical billing, may prove costly to the health care providers. Claims will be declined or postponed more often without pre-checking insurance coverage and benefits, which will result in revenue loss and loss of cash flow. Patients can have an unpleasant surprise, leading to conflicts, frustration, and a lower opinion of the healthcare experience.
On top of that, there is an increment in administrative expenses, as a result of resubmission of claims, manual follow-up with payers, and more time used by the administrative personnel to correct inaccuracies. In general, the lack of verifying the eligibility compromises the revenue cycle management and efficiency.
How iSolve RCM Enhances Eligibility Verification
Eligibility verification in medical billing is necessary to minimize claim denials, billing patients properly and enhance revenue cycle management. Consistent and extensive verification process enables healthcare providers to verify insurance coverage, benefits, and financial responsibility of the patient prior to rendering the services and iSolve RCM can be used to facilitate the process by providing automated eligibility checks, real-time insurance checks, and extensive documenting capabilities to enable medical practices, hospitals, and clinics to ease the process of insurance benefits verification, better claim acceptance, and overall revenue performance. iSolve RCM allows providers to become more efficient in their operations and provide a clear and smooth experience to patients.
FAQs
How is the process of eligibility and verification?
Medical billing eligibility and verification process entails ensuring that a patient is insured, benefits and has the responsibility of the services provided prior to services before services are delivered. It promises active coverage, recognizes copays, deductibles and service restrictions, and prevents claim denials and enhances revenue cycle management of healthcare providers.
What is the meaning of medical verify eligibility?
In medical billing, to ensure that an individual is eligible, one has to confirm their insurance coverage of the patient, the type of the plan, and their benefits prior to treatment. It establishes active coverage, covered services and financial responsibility which allows healthcare providers to make clean claims and prevent reimbursements by insurance payers that were denied or delayed.
How do we check the eligibility of patients?
The steps are as follows:
(1) Obtaining patient demographics and insurance data.
(2) checking active coverage and date of policy.
(3) checking covered services and network status.
(4) determining patient financial responsibility.
(5) checking referrals or prior authorizations.
(6) recording and communicating findings in billing system.
What is an eligibility verification?
Medical billing is the process of verifying the insurance cover of the patient, his or her benefits, and financial liability prior to healthcare services. It assists in verifying that claims are correct, services are covered, and that patients know their copays, deductibles and coinsurance, which will minimize denials and billing errors.
What are the four forms of verification?
Verification is of four common types:
(1) Manual verification is done over the phone or payer portal.
(2) Electronic verification is done using EDI transactions (270/271).
(3) Clearinghouse verification is done through integrated software.
(4) Automated real-time eligibility verification is done via EHR or practice management system.
What is the meaning of eligibility in healthcare?
Within the medical field, eligibility means the ability of a patient to receive insurance coverage in a particular health plan. It also dictates whether services are covered, the range of the benefits and financial responsibility to patients so that healthcare providers can bill correctly and patients know their out-of-pocket expenses.




