Medical billing is an essential practice that helps healthcare practices get reimbursed for the services they render. Effective medical billing collections are important for the cash flow of a healthcare practice. This helps the practice to sustain itself.
The knowledge of collection rate in medical billing and net collection rate in medical billing can be extremely beneficial for medical practices to understand their efficiency in the process and take appropriate measures to increase their collection rates. Average medical billing collection rates help practices measure revenue performance and efficiency. This blog explores billing collection rates and what practices should know, including how a medical billing company in USA supports healthcare providers to improve collections and manage revenue cycles effectively.
What is a Medical Billing Collection Rate?
The collection ratio in medical billing is a term that procedures the efficiency of a practice in collecting payments for services rendered by a practice. It is calculated by dividing the total amount collected by the total amount charged. A high collection ratio means that a practice is well-organized in revenue management.
The net collection rate in medical billing emphases on the actual revenue collected after modifications, write-offs, and denials, associated to total expected payments. Unlike gross charges, which show all billed amounts, the net collection rate reflects accurate earnings, helping practices understand true financial performance and identify areas for improvement.
A major factor for consideration is the percentage of medical billing collections, which represents the portion of the service that was successfully collected. According to a study conducted by the National Institutes of Health (NIH) on medical debt and medical collections within the US, as of 2024, 36% of US households have medical debt, 21% have unpaid medical bills, and there are $194 billion in active medical collections. It is essential for medical institutions to keep track of the percentage of medical billing collections over time to establish trends, assess the staff or service, and improve the service. By tracking the average medical billing collection, the service can improve the billing service.
Pro Tip: Regularly monitor your practice’s average medical billing collection rates and track trends to quickly identify inefficiencies, reduce denials, and optimize overall revenue performance.
Average Medical Billing Collection Rates
The Average medical billing collection rates services differ from one specialty group to another and from one practice size group to another. This helps them benchmark their performance and work on improving their efficiency. Durable average medical billing percentage specifies effective claims management and timely reimbursements.
Industry Benchmarks by Specialty
The medical billing percentage of collections varies depending on the specialty type. For instance, surgical practices may have a higher percentage compared to primary care. On the other hand, specialties like dermatology may have delayed or partial payments.
Small vs. Large Practices
The smaller practices may face difficulties in collecting lower average medical billing revenues due to fewer staff, whereas larger practices can take advantage of technology and staff dedicated to billing services to increase revenues. Practices with higher average medical billing collection rates preserve healthier and stable revenue cycles.
Insurance vs. Self-Pay Collections
It depends on the mix of patients who are insured and those who are self-pay patients. Some medical practices may have a higher number of insurance claims, which may lead to denials, thereby influencing medical billing percentages, while self-pay patients may lead to quicker and more consistent collection, depending on how they are managed.
Benchmarking for Performance Improvement
Monitoring average medical billing collection rates against industry standards supports identifying underperforming areas. This enables practices to take corrective measures such as training staff, improving coding practices, or considering the services of professional medical billing services and medical coding services to enhance accuracy, reduce claim denials, and improve overall revenue cycle performance.
Gross vs Net Collection Rate in Medical Billing
In revenue cycle management, it is important to understand the difference between gross collection rate and net collection rate in medical billing. Both are used to determine the performance of a medical practice based on their collection rate.
The gross collection rate is defined as the percentage of the total charges collected before any contractual adjustment or write-off. To determine the gross collection rate, the total payments made are divided by the total amount billed. The gross collection rate gives an overview of the amount collected compared to the amount billed. Many instances of low collection rates are a result of claim denials. Reviewing common denial codes in medical billing can help practices correct errors and improve success.
The net collection rate in medical billing is defined as the amount collected compared to the expected reimbursement. The net collection rate is considered a better way to determine performance since it does not include any amount that is not expected to be collected.
Pricing Models Explained: Choosing the Right Approach
Learn how various pricing models, percentage-based, per claim, hourly, and flat fee, affect costs, suppleness, and client-provider agreements.
A Percentage of Collections
This type of pricing model charges clients a fixed percentage of funds that are recovered or generated on their behalf. This type of pricing model ensures that the service provider’s incentives are closely aligned with that of the client’s, as they are compensated entirely based on success.
For example, a debt collection service could charge 2.5 percent of recovered debt, or a legal service could charge 6 percent of a recovered personal injury case settlement. This type of pricing model is commonly used in legal services, insurance claims, or financial recovery services.
Per Claim Fees
The per claim fee model involves a client being charged a certain amount for every claim or transaction, regardless of whether the claim or transaction was a success or not. This model provides a client with a predictable cost, which makes it ideal for use by a company that processes a large number of similar claims or applications.
For instance, a company that deals with insurance claims can charge a client $50 for every claim, while a medical billing company can charge a client $10 for every claim submitted.
Hourly Rate
The hourly billing system is based on the actual hours spent working on a particular project or case. This is best suited for projects that are not fixed in terms of complexity or need extensive customization. The cost is directly related to the work done, which makes it transparent but could also affect the overall cost of the service provided.
For example, if we consider a business consultant, his or her cost could be $150 per hour, or if we consider a legal consultant, his or her cost could be $300 per hour for legal services.
Flat Fee
The flat fee model is where a set fee is charged for a given service, irrespective of the time involved. This model provides a predictable fee to the client, making it easier to budget. However, the service providers have to make an accurate estimate to be able to make a profit.
For instance, a law firm may charge a client $1,000 to write a will. Another example is a tax preparation firm charging a client $200 to prepare a tax return. This model works best where the scope of the service is well defined.
Factors Affecting Collection Rates
There are several factors that affect medical billing collections. The factors include insurance denials, patient payments, and coding. The understanding of these factors can help a medical practice minimize losses, optimize medical billing charges, and manage medical billing costs.
Insurance Claim Denials
Insurance claim denial has a major impact on medical billing collection. It delays the payment and creates additional work. Monitoring and follow-up on a regular basis help reduce denial rates. This helps in faster payment.
Follow-Up Processes
Effective follow-up on pending claims is a critical activity. Medical practices that track the statuses of the claims they send out tend to maintain a high rate of medical billing collections. This minimizes revenue loss.
Patient Payments and Self-Pay Balances
Unpaid patient balances can reduce the overall collection. Clear billing statements, patient payment plans, and timely reminders can help to improve the medical billing charges collected from self-pay patients.
Accuracy of Medical Coding
Incorrect coding can result in denied or delayed claims. The impact of such errors can be realized in the medical billing costs. Precise medical billing and coding can assist in efficient claim processing.
Staffing and Process Efficiency
Understaffed or disorganized billing operations can delay the process. Efficiency in workflow, training staff, and utilizing technology or outsourcing to professional medical billing services can increase efficiency and minimize errors in the process and maximize medical billing collection.
Pro Tip: Regularly review insurance denials, patient balances, and coding accuracy. Streamline workflows, train staff, and consider leveraging technology or outsourcing to a professional medical billing service to maximize revenue collections while minimizing errors.
How to Calculate Collection Rate
The collection ratio is a key figure in medical billing that measures the efficiency of a practice in collecting payments for services rendered. It is used to determine the efficiency of a practice. Tracking average medical billing collection rates supports reduced denials and advanced financial outcomes.
Here are following Step-by-Step Calculation:
- Total Collected – Add all payments received from insurance companies and patients for a given period.
- Total Charges – Sum all charges billed for the same period.
- Apply the Formula:
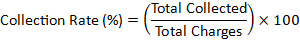
Example 1:
Total Charges: $120,000
Total Collected: $100,000
Collection Rate = (100,000 ÷ 120,000) × 100 = 83.3%
Example 2:
Total Charges: $50,000
Total Collected: $42,500
Collection Rate = (42,500 ÷ 50,000) × 100 = 85%
Medical practices are able to evaluate their performance, set genuine targets, and identify the areas that require improvement in their systems by monitoring this figure on a regular basis. It is indispensable for a medical practice to know how to calculate the collection rate in order for them to be successful.
Common Reasons for Low Medical Billing Collection Rates
Healthcare practices face the challenge of low medical billing collections due to various reasons. Understanding the causes will help the healthcare practice enhance the efficiency of the revenue cycle.
One of the causes is the denial of medical claims due to coding errors, insufficient documentation, or the lack of prior authorizations. This affects the timely payment of the medical bills. There is a need to follow up on the denied claims to ensure timely payment.
Another cause is the delay in submitting the medical claims or the inability to follow up on the unpaid medical bills. This will result in low medical bill collections. Improving the efficiency of the medical billing will enhance the revenue cycle. Additionally, practices should also monitor their accounts receivable, as delayed payments will impact collection performance. Understanding AR in medical billing will help identify unpaid claims, which will improve efficiency in the revenue cycle.
Improving Your Medical Billing Collection Rates
For optimizing the collection of medical billing, the areas to focus on are reducing denial, patient payments, technology, and outsourcing. The knowledge of the cost of a medical billing service, as well as the medical billing pricing strategy, can aid the maximization of revenue.
Reduce Claim Denials
Denials are the reasons for delays in payments and affect complete collections. Guaranteeing accurate coding, authenticating the patient’s insurance eligibility, and submitting comprehensive documentation can minimize denials. Using effective denial management services can further help identify and resolve claim issues quickly. This advances medical billing collection.
Follow Up on Pending Claims
Timely developments on unpaid claims can avoid loss of revenues. An organized tracking system can be executed to confirm timely complements on unpaid claims, in so doing maintaining high efficiency in collection.
Improve Patient Payment Processes
Deliver clear billing statements, stretchy payment plans, and possibilities for making payments online. Efficient patient balance management is an important step to boost medical billing collection efforts
Leverage Technology
The use of electronic health records (EHRs) and computerized billing software can also support update claims, reduce errors, and track collections. Technology also assists in accurate medical billing pricing.
Consider Outsourcing
Partnering with professional collection billing services can support upsurge efficiency, reduce organizational load, and improve medical billing collection. Outsourcing is commonly a cost-effective approach compared to in-house teams.
Monitor and Adjust Service Rates
Medical billing service rates and pricing models need to be regularly evaluated to ensure that they are aligned with industry standards and are profitable while also maintaining competitive pricing for medical billing services.
How Much to Charge for Medical Billing Services
Normally, medical billing services are either charged on a percentage basis of collected revenue or on an hourly basis. In case you are thinking about how much should I charge for medical billing services, then it is a general consensus that the charge may vary from 4% to 10%, depending on the collected revenue.
Other service providers may use the hourly rate, not the percentage system. The average hourly rate for a medical billing and coding company can range from $20 to $65. The knowledge of these systems will aid a medical practice in making a well-informed decision regarding the cost of the medical billing service. The average medical billing and coding company charge per hour normally ranges from $20 to $65 that depend on expertise, service scope, and geographic position.
Pro Tip: When establishing fees for your medical billing services, consider your practice size, claim volume, and complexity. Decide between a percentage-based or hourly billing system that is competitive, profitable, and fair.
How iSolve RCM Support with Collection Rates
Effective revenue management is critical for ensuring that a healthcare practice has a steady stream of income. iSolve RCM helps healthcare providers achieve this by ensuring timely and accurate medical billing collection, clear medical billing rates, and flexible medical billing services pricing. This helps them improve their financial position by increasing revenue growth.
Frequently Asked Question’s
What percentage do most medical billing companies charge?
The average medical billing firms will charge 4-10 percent of the total collections. The definite rate is conditional on the practice size, the quantity of claims, the complexity of the specialties, and the presence of such services as the coding, denial management, and full revenue cycle management.
What is a good gross collection rate in medical billing?
An adequate collection rate in medical billing is 90 per cent and above. This rate compares the percentage of the total charges billed that have been collected before adjustments and reflects the efficiency at which the payment is gathered by a practice.
What happens if a $200 medical bill goes to collections?
When a medical bill of 200 dollars is sent to collections the medical provider can send the bill to a collection agency. It would have an impact on credit reports, recurring payment requests, and even extra fees.
What is considered a good collection rate?
It is typical to obtain a good collection rate in healthcare billing between 95-98% of the net collection. Good performing practices have good billing procedures, proper coding and follow-ups in order to ensure that they maximize on the reimbursements.
What are the top 5 denials in medical billing?
Some of the common medical billing denials entail misinformation of the patient, absenteeism of documentation, inadequate prior authorization, coding mistakes, and insurance non-coverage services. These issues are solved to enhance claim acceptance and general efficiency of the revenue cycle.
What is the most common rejection in medical billing?
Wrong insurance ID or demographics most often fix the rejection of claims in medical billing because of misconstrued or lacking patient information. Such mistakes lead to the rejection of claims before processing and the rebates taking longer to come about after they are corrected and resubmitted.




