Authorization in medical billing represents a key element in the contemporary healthcare reimbursement system, which acts as a precursor for approval by the insurer prior to the provision of certain medical services. This process creates a structured approach for evaluating medical necessity, cost control, and compliance in the healthcare revenue stream.
This blog offers an analytical overview of authorization in medical billing, which includes the definition, importance, and role of insurance providers in medical billing authorization. Additionally, the blog delves deeper into the process, different types, and challenges of authorization, along with the premeditated practices for medical billing authorization by a medical billing company in USA.
What is Medical Authorization
A medical authorization is a structured approval method for healthcare billing. This method ensures the medical service meets the insurance requirements before providing the treatment. Knowing what is medical authorization can provide a better explanation for what is authorization in medical billing by determining whether the medical service is necessary.

How Medical Authorization Works
The process starts with the providers making a request along with the necessary clinical information to the insurance for evaluation. In medical billing, the workflow may involve a pre-authorization in medical billing and a prior authorization in medical billing.
Who Requires Medical Authorization
In medical authorization, there are several stakeholders, including patients, service providers, and insurance companies. The service providers are the initiators, insurance companies verify medical necessity, and patients are required to wait for approval. This is also consistent with insurance authorization in billing systems, ensuring services are provided appropriately.
Pre-authorization, also known as prior authorization, prior approval, or precertification, is a decision made by insurance companies regarding their determination of whether a healthcare service, treatment plan, medication, or durable medical equipment is actually medically necessary. According to the Centers for Medicare & Medicaid Services, some services require pre-authorization prior to delivery, unless it is an emergency. Pre-authorization is not a guarantee of coverage, as documentation is critical in medical billing.
Key Components of Medical Authorization
These key components may include information about the patient, clinical documentation, procedure information, and approval status. Data accuracy prevents denial of authorization in medical billing processes and enhances the acceptance rate for different types of authorization in medical billing.
What is Insurance Authorization in Medical Billing
Insurance authorization is the insurer’s official approval, which approves that a proposed service is both necessary and insured. It guarantees compliance with billing requirements, safeguarding both patients and service providers from unexpected costs or claims rejection.
The difference between medical authorization and insurance authorization can be understood in terms of scope, where medical authorization commonly refers to the process of approval, as opposed to insurance authorization, which exactly involves validation prior to service delivery, confirming appropriate documentation and verification of medical necessity.
Authorization of insurance is required for costly procedures, surgeries, tests, or treatments. This helps prevent delays in claims and ensures that there is no denial of claims during medical billing. This is helpful for the revenue cycle of healthcare.
Pro Tip: Always verify insurance requirements and obtain authorization in advance to prevent claim denials and confirm a smooth revenue cycle.
Types of Authorization in Medical Billing
Authorization plays a vital role in medical billing as it ensures that medical services are authorized by the insurance companies before they are delivered. The different types of authorization in medical billing assist medical service providers in streamlining medical claims.
Pre Authorization (Prior Authorization)
Pre-authorization in medical billing, as a process, seeks approval from the insurance firm before undertaking certain medical procedures or services. This ensures that the medical procedures are necessary and that they are covered.
Prior authorization, according to the American Medical Association, is a cost control process used by health plans that requires providers to qualify for payment before providing a service. Although prior authorization can be useful in ensuring that a service is necessary, in practice, it can be overused, costly, inefficient, and opaque, leading to undue delays in patient care.
Concurrent Authorization
Concurrent authorization, on the other hand, is carried out during a course of treatment or hospitalization. This ensures that continued care is medically necessary, allowing insurers to keep a check on costs and compliance while the treatment progresses, thus avoiding denial of authorization in medical billing.
Retrospective Authorization
On the other hand, retrospective authorization occurs after the provision of care, usually in emergency or unplanned procedures. The insurance companies assess the documents retrospectively to ascertain coverage. This ensures medical necessity and adjusts the payment while protecting the service providers from possible disputes over claims.
Referral Authorization
Authorization for referral is a requirement when a primary care physician recommends a specialist or outside service. It verifies that the insurance company has approved and included coverage for consultations, tests, or treatments in order to ensure that the patient gets the care that is needed while still being in accordance with the insurance authorization requirement.
Pre Authorization (Prior Authorization) in Medical Billing
Pre-authorization in medical billing is defined as the process where the insurance company provides prior authorization for a particular service before the service is rendered. This is a crucial step in the efficient management of the revenue cycle in the healthcare industry.
Prior authorization in medical billing can be related to the term pre-authorization, which also calls for a review by the insurer before treatment can take place. The terms used might differ from one insurer to another, and the process can help in the compliance of medical billing with the rules set by the insurer, avoiding delays, and denial of authorization.
Authorization is also required for high-cost services such as procedures, imaging tests, surgeries, or visits with a specialist. This process includes the submission of the documents, the process by the insurance company, and the authorization process. Although this process increases the accuracy of claims, some challenges are encountered, for example, in terms of delay, information, and communication; hence, the significance of what is pre-authorization in medical billing is emphasized.
Pro Tip: Confirm all documentation is complete and precise, submit pre or prior authorization promptly, and maintain clear communication to avoid delays and claim denials.
What is an Authorization Number in Medical Billing?
An authorization number is a unique identifier issued by the insurance company upon approval of the medical service. This verifies the insurance coverage and tracks the approval procedure. Proper utilization of the authorization number by the healthcare providers can help them avoid denied claims and efficiently manage the revenue cycle.

How Authorization Numbers Are Generated
Authorization numbers are created during the review process undertaken by the insurance company for a pre or prior authorization request. The system provides a unique authorization code that is related to the information regarding the patient and the procedure that has been approved. Proper generation provides traceability for the process so that errors are avoided during claims processing.
Importance of Authorization Number in Claims
The authorization number serves as a proof of approval by the insurer. The inclusion of this information in the claims ensures that authorization denial is avoided, thus promoting faster reimbursement and a verifiable audit trail. Therefore, this information is a crucial part of revenue management.
Where to Use Authorization Number in Billing
Authorization numbers should be included on claim forms, electronic claims, and patient records. They are referenced during the process of eligibility, billing reconciliation, and auditing. The use of authorization numbers is crucial for the smooth processing of claims and the prevention of denied claims.
Best Practices for Handling Authorization Numbers
Keep track of authorization numbers, verify them before billing, and track expiration dates. Inclusion of numbers in billing software can help in minimizing errors, ensuring compliance with insurance, and improving the efficiency of the revenue cycle in medical billing.
Authorization Denial in Medical Billing
Authorization denial occurs or happens when an insurer denies approval for a service that a person wants or requests. This can cause a delay in service, a halt in revenue, and a need for corrective action.
What is Authorization Denial
Authorization denial occurs when the insurer denies approval for a service due to non-fulfillment of coverage criteria, lack of documentation, or policy constraints. Knowing about authorization denial in medical billing can help medical providers take care of claims in a timely manner, so that they are not surprised by a loss in revenue.
Common Reasons for Authorization Denial
Denials can also occur due to incomplete paperwork, outdated information, issues of medical necessity, and incorrect coding during the procedure. Incorrect coding is another aspect of the significance of professional medical coding services. In addition, lack of preauthorization in medical billing can also lead to denials, which can affect the provider-patient relationship.
Impact of Authorization Denial on Revenue Cycle
On the other hand, authorization denial may cause a delay in the reimbursement process. Each denied authorization requires further verification, resubmission, and appeals. This may impact the efficiency of the healthcare revenue cycle and may result in the rejection of claims.
How to Prevent Authorization Denial
Denials may also be avoided through ensuring that the patient is eligible, providing complete documentation, abiding by the insurer’s guidelines, and procuring pre or prior authorization. Denial management services, along with training employees, help in averting errors, enhancing accuracy, and saving financial losses.
Steps to Resolve Authorization Denial
Feedback from insurers, correction of missing or incorrect data, resubmission of requests, and communication with patients and insurers are necessary, to address a denial. Timely follow-up is grave in overturning denials and receiving proper reimbursement.
Authorization Workflow in Medical Billing
The authorization process provides a structured process for seeking authorization from the insurer prior to receiving medical services. This procedure is also beneficial for ensuring compliance, reducing denials, and restructuring claims. A clear process is compulsory for appropriate documentation and revenue cycle management in healthcare billing.
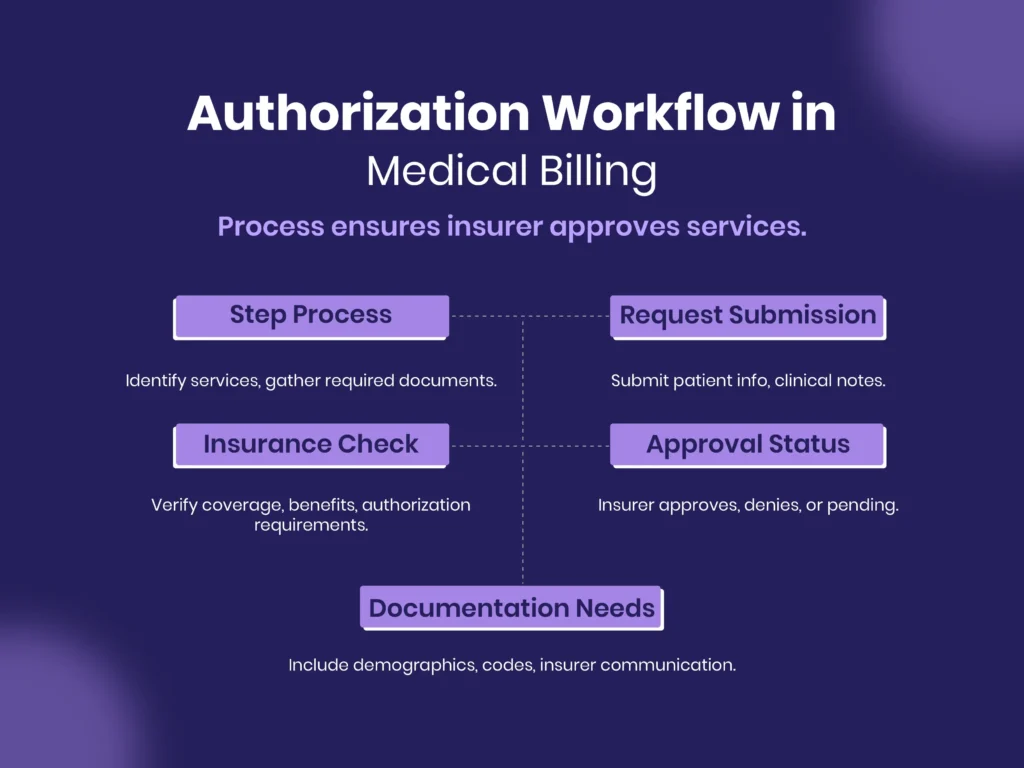
Step-by-Step Authorization Process
The step-by-step procedure for authorization starts by identifying the services to be authorized, obtaining clinical documentation, making insurance requests, and tracking the response. Knowledge of the types of authorization is necessary for medical billing practitioners to follow a standard procedure for authorization.
Insurance Verification and Eligibility Check
Insurance verification ensures that the patient has coverage and benefits, while eligibility verification ensures that the service for which the patient seeks authorization does not require authorization. These steps are taken in advance, which ensures compliance and prevents pre-authorization issues in medical billing.
Insurance verification validates the insurance coverage and benefits for the patient, while insurance eligibility verification verifies whether the insurance requires authorization. Carrying out this procedure before the eligibility verification process in medical billing is crucial for compliance purposes and avoids pre-authorization problems.
Submission of Authorization Request
This process of submitting an authorization request entails providing the insurer with the patient’s information, clinical notes, and procedural codes. This process is very important in order to avoid any errors, thus promoting a smooth process for claim handling in medical billing.
Approval, Pending or Denial Status
The insurer either approves, denies, or makes a pending decision on the claim, once the submission is made. Approvals facilitate service continuation, whereas denials or pending require further action. Effective tracking ensures that denial in medical billing authorization is minimized.
Documentation Requirements
Documentation may include the demographic information of the patient, clinical notes, procedure codes, and communication with the insurer. This will ensure compliance with the requirements of the insurer, auditing, and verification of claims, thus avoiding any disruption in revenue.
Pro Tip: Accurate patient and clinical documentation, advance verification of eligibility, tracking of all authorization requests, and follow-up activities are some of the best practices that help ensure a smooth healthcare revenue cycle.
Best Practices for Managing Authorization in Medical Billing
The management of authorizations in medical billing is noteworthy for reducing denials, certifying compliance, and modernizing claims. The application of best practices would advance efficiency, boost revenue cycle performance, and confirm provider reimbursement. Following are the key practices for authorization in medical billing:
- Patient eligibility should be verified before sending in any type of request for pre-authorization in medical billing.
- Complete clinical information should be collected in order to avoid denial of authorization in medical billing.
- Authorization requests should be sent in a timely manner in order to avoid delays in the approval process from the insurer.
- All types of authorization in medical billing should be well understood by the staff.
- All approvals, denials, and pending requests should be well documented in medical billing.
- Automated tools should be used for keeping track of authorization numbers and deadlines for sending in requests.
- Changes in the services that are covered should be kept track of in the insurer’s guidelines.
- Patients should be kept abreast of the situation regarding approvals.
- The authorization process should be audited from time to time in order to identify gaps in the process.
- Follow-ups on pending or denied requests should be made in a timely manner in order to avoid delays in medical billing.
How iSolve RCM Supports Authorization in Medical Billing
iSolve RCM is modernizing the way authorization management is handled by automating the process of eligibility verification, pre and prior authorization, and tracking the status of the approval process. It also minimizes errors, prevents denial of authorization in medical billing, and ensures timely reimbursement, thereby maximizing the revenue cycle process efficiently.
Frequently Asked Questions
What is authorization in medical terms?
Authorization refers to the insurer’s approval for a medical service before the service is rendered, In medical terminology. This is done to confirm coverage, verify the medical need for the service, and avoid unexpected expenses for the insured individuals and healthcare providers.
Does Mounjaro require prior authorization?
Yes, Mounjaro needs prior authorization for insurance coverage. Providers must also deliver medical documentation that justifies the medical necessity for the drug, the eligibility of the patient for coverage, and the requirements for coverage before the drug is actually dispensed to the patient to minimize the risk of denial.
What is billing authorization?
Billing authorization is a type of approval from the insurer, which validates whether a service is covered or not before billing occurs. This process ensures that appropriate documentation takes place, medical necessity is verified, and denial of authorization does not take place in medical billing.
What is authorization in simple words?
Authorization is an approval from an insurance company for a healthcare service. It is a confirmation of whether or not it is necessary for a patient and whether or not it is covered. It helps patients avoid surprise bills.
What are the three types of authorization?
There are three major categories of authorization, namely: pre-authorization, which is before the provision of the services; concurrent authorization, which is during the course of treatment; and retrospective, which is after the provision of the services.
What is without authorization?
“Without Authorization” means a medical service is provided without prior insurer authorization. A service provided without prior authorization may not be reimbursed, resulting in increased financial responsibility for the patient, and denial of services during medical billing.




